Uveitis And Eye Inflammation
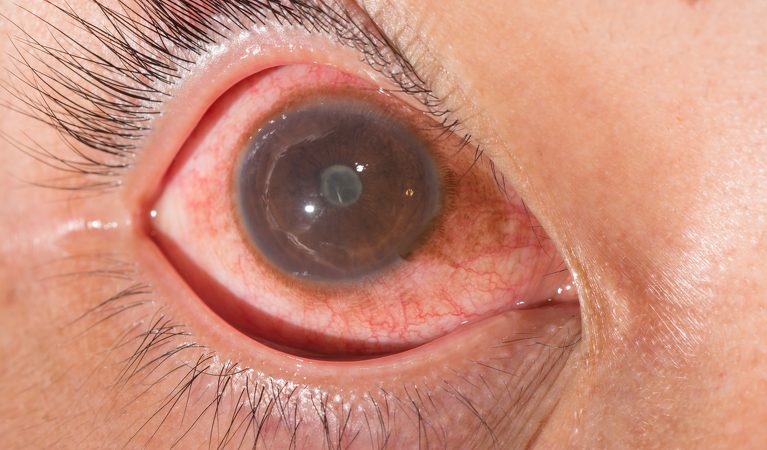
What is Uveitis?
A sheath of 3 layers surrounds the gel-like substance at the center of the eyeball. The middle layer is called the “uvea”. Inflammation of the uvea is called “uveitis“. Uveitis may affect any or all of the layers called the iris, choroid and ciliary body, the three of which are named the uvea together.
The uvea is now considered a separate field of speciality for eye doctors. The diagnosis and treatment of uvea-related diseases are increasingly supported by developments in immunology (science of immunity) and genetics.
The most important factors in successful treatment are early diagnosis, collaboration between the doctor and patient, and accurate therapy. The damaged eye can be saved most of the time if these conditions are met.
Even if the treatment is completed, the patient should be monitored at least every three months. Since the disease can recur without being noticed, control visits should not be missed. The ophthalmologist should be informed about any different signs of other organs. For example, aphthae in the mouth, spots on the skin, rheumatic symptoms etc.
Uveitis is a very complicated disease and may have a different course in every patient. Treatment is unique for every person, as is the course of disease. It is essential that the drug dose to be used for treatment is determined by experienced doctors who are specialized in the uvea.
Causes of Uveitis
The cause of disease cannot be exactly determined in 30-40% of patients with uveitis. Uveitis can develop due to factors like viruses, fungus and parasites or occur as an ocular sign of another disease. Therefore, diseases should be investigated with various tests. Uveitis may also develop concomitantly with systemic diseases originating from collagen tissue and of autoimmune origin. Examples include Behçet’s disease, ankylosing spondylitis and rheumatoid arthritis.
Disorders which may cause uveitis:
- Behçet’s disease
- Infections (bacterial, viral, parasitic or fungal) can spread to the eyes from other areas. Tuberculosis, syphilis, herpes, toxoplasmosis etc.
- Ocular trauma and surgeries
- Autoimmune reactions (diseases of the immune system), rheumatoid diseases, ulcerative colitis, sarcoidosis.
Symptoms of Uveitis
When it forms in the front part of the eye, the symptoms of uveitis include redness in the eye, blurred vision, pain around the eye, oversensitivity to light and eye floaters. If uveitis is mainly localized in the rear part of the eye, blurred vision is the most common symptom. If uveitis involves the visual center, sudden reduction of vision and loss of vision due to tissue damage occurs. The main symptoms of uveitis developing outside the central region include:
- Eye redness
- Watering of the eyes
- Light sensitivity and glare
- Spotty and blurry vision or severe loss of vision
- Sudden flashes
- Pain in the eyeball
Types of Uveitis
- Anterior
- Intermediate
- Posterior
Stages of Ophthalmic Examination
How Is Uveitis Diagnosed?
Regardless of its severity, uveitis is an urgent disease. The disease progresses if intervention is delayed, and may leave permanent side effects due to inflammation, such as pupillary deformities, cataract and elevated ocular tension. The first thing to do when symptoms start is to consult an ophthalmologist experienced in uveitis. If the patient is late having the first examination, vision may be lost permanently.
Certain types of uveitis have a typical appearance and can be diagnosed immediately. Even in such cases, advanced techniques such as angiography, ultrasonography and ERG may be required to find out the extent to which vision is at risk and to monitor the efficacy of treatment, if the rear part of the eye is involved. For instance, angiography performed with a dye called ICG (indocyanine green) can provide definite diagnostic information about the disease in suspected cases. Rheumatologists, pulmonologists, dermatologists and neurologists can then collaborate for joint investigation.
Behçet’s disease is a disease which is characterized by recurrent aphthous wounds in the mouth and genitals and causes uveitis. However, Behçet’s disease is a chronic inflammatory disease which may involve almost all bodily systems, joints, larger and smaller vessels, the central nervous system and organs of the digestive system. The signs and symptoms of the disease present as exacerbations in the involved organs and, while some symptoms are long-lasting, there are periods when the patient has no lesions or complaints, which vary from person to person.

